
TL;DR:
- Autism support varies based on individual needs, location, funding, and policies.
- Regional disparities and provider shortages significantly impact access and wait times.
- Family advocacy and informed navigation are crucial for obtaining personalized, effective services.
Finding the right support for your child with autism can feel like solving a puzzle with missing pieces. One family gets 30 hours of weekly therapy, another gets 10. One town has four specialized clinics, the next has none. This isn’t random, and it’s not unfair by accident. Autism services differ because every child’s needs are unique, every state’s funding looks different, and every community’s resources are limited in their own way. This guide breaks down exactly why these gaps exist, what drives them, and what you can do to navigate the system confidently and get your child the right support.
Table of Contents
- How individual needs shape autism support
- Why location matters: Regional and resource gaps
- The influence of funding, insurance, and policy
- Different philosophies and family advocacy
- Our perspective: What most guides miss about navigating autism services
- Find personalized autism services near you
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Services are individualized | Support varies based on each child’s needs and clinical benchmarks, not just diagnosis. |
| Geography impacts access | Location determines what services, providers, and therapies are realistically available. |
| Policy shapes resources | Insurance mandates and Medicaid funding drive major differences in service coverage. |
| Family advocacy matters | Active, informed advocacy helps close access gaps and secure better support. |
| Evidence matters most | Prioritize effective, individualized, and evidence-based strategies over chasing the latest trend. |
How individual needs shape autism support
Every child on the spectrum is different in ways that go far beyond a single diagnosis. The type and intensity of support your child receives starts with their individual profile, assessed through clinical tools that look at communication, behavior, and daily living skills.
The DSM-5 support levels classify autism into three tiers, and these tiers directly influence what services are recommended. A child at Level 1 may need targeted social skills coaching and some school accommodations. A child at Level 3 may need intensive, round-the-clock support across multiple settings. Autism services vary primarily because of these individual differences in need, assessed through those DSM-5 classifications.
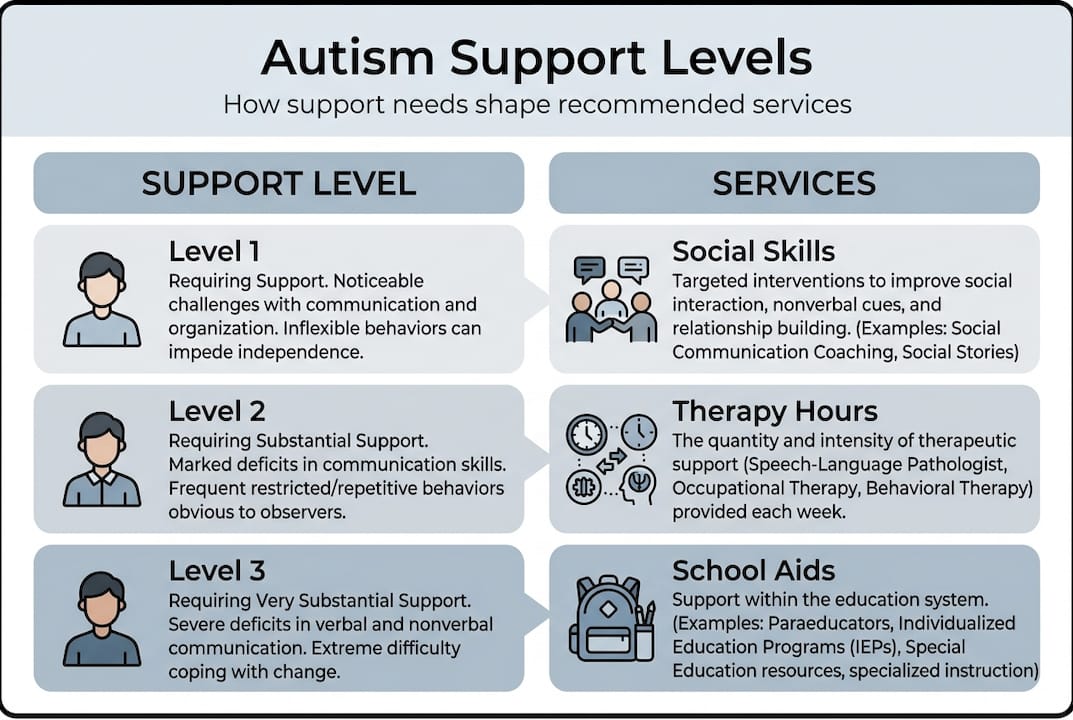
Once a support level is established, the specific therapy approach matters just as much. Applied Behavior Analysis (ABA) focuses on building measurable skills through structured reinforcement. Occupational therapy targets daily living skills like dressing, writing, and sensory regulation. Speech therapy addresses communication from single words to complex conversation. Each of these is matched to what the child actually needs, not a one-size-fits-all prescription.
The research behind this is important to understand. ABA is effective for improving adaptive skills with a standardized mean difference of 0.51, but effectiveness varies significantly based on each child’s starting point. A child who is already verbal will respond differently to language-based therapy than a child who is pre-verbal. This is why two children with the same diagnosis can be in completely different programs.
Key factors that shape your child’s service plan:
- Current communication level (verbal, minimally verbal, or non-verbal)
- Sensory processing patterns and sensory sensitivities
- Cognitive and adaptive functioning scores
- Age at the time of diagnosis and intervention start
- Presence of co-occurring conditions like ADHD or anxiety
| Support Level | Typical Services | Session Intensity |
|---|---|---|
| DSM-5 Level 1 | Social skills groups, school support | Low to moderate |
| DSM-5 Level 2 | ABA, speech, OT combined | Moderate to high |
| DSM-5 Level 3 | Intensive ABA, specialized school | High to very high |
Pro Tip: When identifying tailored programs for your child, bring a detailed written summary of their daily strengths and challenges to every evaluation. Clinicians can build more accurate plans when they see the full picture, not just test scores.
Why location matters: Regional and resource gaps
Your zip code has more power over your child’s services than most people realize. While individual needs define what support would be ideal, geography determines what’s actually within reach.
In the United States, access to autism services is dramatically uneven. States like Colorado and Massachusetts have robust provider networks, strong insurance mandates, and well-funded early intervention programs. Others, like West Virginia, have far fewer specialists, longer wait times, and thinner community resources. Disparities in autism services across US states and countries like Germany and Spain versus Poland show that geography can determine service quality as much as any clinical factor.
The gap between urban and rural areas within states is equally stark. A family in Denver may wait six weeks for an ABA evaluation. A family 90 miles away in a rural county may wait 18 months for the same appointment. Provider shortages, fewer trained therapists, and limited clinic infrastructure all compound in rural settings.
Why gaps form in certain locations:
- Shortage of trained behavior analysts and speech-language pathologists
- Lower reimbursement rates discouraging providers from rural practice
- State-level differences in Medicaid coverage and school funding
- Limited transportation infrastructure for families without reliable vehicles
- Fewer university programs producing autism specialists in certain regions
The international picture is even more varied. Families in Germany can access publicly funded early intervention with relatively short timelines. Families in Poland or parts of the UK face dramatically longer waits. In fact, 81% of UK referrals wait five or more years for autism services. That’s not a minor inconvenience. That’s children missing critical early intervention windows.
| Region | Typical Wait Time | Key Resource Factor |
|---|---|---|
| Colorado, USA | 6 to 12 weeks | Strong insurance mandate |
| West Virginia, USA | 12 to 24 months | Provider shortage |
| Germany | 3 to 6 months | Public funding model |
| UK (NHS) | Up to 5 or more years | Underfunded referral system |
Understanding insurance mandates for autism support in your state is one of the most practical steps you can take. And navigating local service systems effectively often means knowing which agencies to contact and in what order.
The influence of funding, insurance, and policy
Beyond location, public policy and insurance coverage can make or break your options for autism support. These aren’t background details. They are the framework that decides whether a therapy is covered, how many sessions are allowed, and whether a provider even accepts your plan.

In the United States, insurance mandates for autism therapy vary by state. Some states require comprehensive ABA coverage with no session caps. Others allow insurers to set strict annual limits or require prior authorization for every service block. Medicaid eligibility also creates major differences, especially for families with lower incomes who rely on it as their primary coverage.
The numbers behind this are striking. Medicaid ABA spending exploded by 561% in some states, triggering policy reviews, fraud investigations, and rate reductions that rippled through provider networks. Rapid spending growth drew scrutiny that led to service disruptions for families who had nothing to do with any misuse.
These policy shifts create unpredictability. A family whose child had 30 approved hours per week may suddenly face a cap of 20 hours after a state reauthorization review. Providers may exit the Medicaid network entirely if reimbursement rates drop too low.
Steps families can take to protect their coverage:
- Request a written summary of your insurance plan’s autism benefits each year.
- Ask your provider about prior authorization timelines before starting services.
- Keep records of every session, every approval, and every denial letter.
- Contact your state’s insurance commissioner if a denial seems inconsistent with state law.
- Connect with a patient advocate or autism family organization that knows your state’s rules.
“Knowing your rights is not optional. It’s one of the most protective tools a family can have when navigating a system that changes often.”
Understanding state insurance and Medicaid coverage before you start services saves enormous time and stress later. It also helps to know what to ask providers about coverage from the very first appointment.
Pro Tip: Always confirm whether a provider is in-network before scheduling an evaluation. Out-of-network costs can be three to five times higher, and appeals processes can take months.
Different philosophies and family advocacy
Policy and funding often set the outer limits, but therapeutic philosophies and how actively families advocate further shape which services children actually receive.
There is a genuine debate among practitioners about the best approach to autism intervention. Behavioral versus developmental approaches like ABA compared to Floortime represent two different philosophies. ABA targets specific, measurable skills using structured reinforcement. Floortime, a relationship-based developmental model, prioritizes emotional connection and child-led interaction. Neither is universally right. The fit depends on the child.
The neurodiversity movement adds another layer. Many autistic self-advocates and some clinicians argue that the goal should be accommodation and quality of life rather than pushing children toward neurotypical benchmarks. This perspective increasingly influences how some schools and therapists design their programs.
Families play a larger role in this than most realize. Parents who ask questions, attend IEP meetings fully prepared, and push back on generic plans often get better results. Not because the system rewards persistence unfairly, but because individualized advocacy fills gaps that overwhelmed systems leave open.
What advocacy actually looks like in practice:
- Attending school meetings with written notes and specific requests, not general concerns
- Requesting independent evaluations when school assessments feel incomplete
- Building relationships with providers who communicate openly and explain their reasoning
- Joining parent networks in your area to learn which services others have successfully accessed
- Blending approaches when evidence and your child’s response support doing so
Advocating for individualized support is a skill that families can build over time. And supporting your child’s growth across settings requires consistency between what happens in therapy and what happens at home.
Our perspective: What most guides miss about navigating autism services
Most articles about autism services focus on what’s available. We want to talk about what actually works for families navigating this in real life.
The biggest trap we see is the assumption that more is always better. Intensity matters, but fit matters more. A child receiving 40 hours per week of therapy that doesn’t match their profile is not better served than a child receiving 15 hours that does. The focus should be individualized, evidence-based plans rather than chasing maximum session hours or the most talked-about approach of the moment.
Families should also stay alert to misleading service claims. Not every provider with a credential is delivering quality care. In high-spending areas especially, some programs have grown faster than quality controls can follow.
The practical wisdom that rarely appears in guides: build your network early. Connect with other families, keep detailed records of every evaluation and report, and communicate proactively with every provider involved in your child’s care. When you are coordinating therapies effectively, the information you share across providers is often what prevents gaps and redundancies.
Waitlists and provider shortages are real. Creativity and persistence within that reality are your most underrated tools.
Find personalized autism services near you
Understanding why services vary is a powerful first step. The next step is finding the right ones for your child. At Autism Doctor Search, we maintain a current and complete directory of autism resources across every major service category, including ABA therapy, occupational therapy, special education schools, mental health services, and more. Browse the autism therapy services directory to find evaluated providers near you. You can also explore options like The Missing Piece ABA Therapy or search the full Autism Doctor Search database to compare providers, read listings, and take the next step with confidence.
Frequently asked questions
Why is there such a long wait for autism services in some areas?
Service wait times are often long in under-resourced areas because there are fewer trained providers and high demand from families. In fact, 81% of UK referrals wait five or more years, which reflects a shortage problem common across many regions.
Does a higher therapy intensity always mean better outcomes for my child?
Not always. The right approach matched to your child’s specific profile matters more than sheer hours. ABA effectiveness varies significantly based on each child’s starting abilities and characteristics.
What should I ask about my insurance coverage for autism therapy?
Ask about session limits, prior authorization requirements, out-of-pocket costs, and which specific therapies are covered. State laws and mandates shape what insurers must cover, so knowing your state’s rules gives you a stronger starting position.
How can families advocate for more or better services?
Families can build knowledge, join local and national advocacy groups, document their child’s needs in writing, and communicate directly with schools and providers. Family advocacy drives access and can overcome systemic barriers when families are informed and persistent.




